Abstract
Objective
To prospectively evaluate the clinical course of patients with severe aortic stenosis (AS) and identify factors associated with treatment selection and patient outcome.
Methods
Patients diagnosed with severe AS in the Rotterdam area were included between June 2006 and May 2009. Patient characteristics, echocardiogram, brain natriuretic peptide (NT-proBNP), and treatment strategy were assessed at baseline, and after 6, 12, and 24 months. Endpoints were aortic valve replacement (AVR) / transcatheter aortic valve implantation (TAVI) and death.
Results
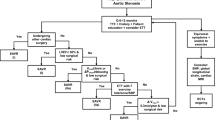
The study population comprised 191 patients, 132 were symptomatic and 59 asymptomatic at study entry. Two-year cumulative survival of symptomatic patients was 89.8 % (95 % CI 79.8–95.0 %) after AVR/TAVI and 72.6 % (95 % CI 59.7–82.0 %) with conservative treatment. Two-year cumulative survival of asymptomatic patients was 91.5 % (95 % CI 80.8–96.4 %). Two-year cumulative incidence of AVR/TAVI was 55.9 % (95 % CI 47.5–63.5 %) in symptomatic patients. Sixty-eight percent of asymptomatic patients developed symptoms, median time to symptoms was 13 months; AVR/TAVI cumulative incidence was 38.3 % (95 % CI 23.1–53.3 %). Elderly symptomatic patients with multiple comorbidities were more likely to receive conservative treatment.
Conclusions
In contemporary Dutch practice many symptomatic patients do not receive invasive treatment of severe AS. Two-thirds of asymptomatic patients develop symptoms within 2 years, illustrating the progressive nature of severe AS. Treatment optimisation may be achieved through careful individualised assessment in a multidisciplinary setting.



Similar content being viewed by others
References
Nkomo VT, Gardin JM, Skelton TN, et al. Burden of valvular heart diseases: a population-based study. Lancet. 2006;368:1005–11.
Faggiano P, Antonini-Canterin F, Baldessin F, et al. Epidemiology and cardiovascular risk factors of aortic stenosis. Cardiovasc Ultrasound. 2006;4:27.
Bonow RO, Carabello BA, Chatterjee K, et al. ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (writing Committee to Revise the 1998 guidelines for the management of patients with valvular heart disease) developed in collaboration with the Society of Cardiovascular Anesthesiologists endorsed by the Society for Cardiovascular Angiography and Interventions and the Society of Thoracic Surgeons. J Am Coll Cardiol. 2006;48:e1–148.
Vahanian A, Baumgartner H, Bax J, et al. Guidelines on the management of valvular heart disease: the Task Force on the Management of Valvular Heart Disease of the European Society of Cardiology. Eur Heart J. 2007;28:230–68.
Lichtenstein SV, Cheung A, Ye J, et al. Transapical transcatheter aortic valve implantation in humans: initial clinical experience. Circulation. 2006;114:591–6.
Litmathe J, Feindt P, Kurt M, et al. Aortic valve replacement in octogenarians: outcome and predictors of complications. Hellenic J Cardiol. 2011;52:211–5.
Smith CR, Leon MB, Mack MJ, et al. Transcatheter versus surgical aortic-valve replacement in high-risk patients. N Engl J Med. 2011;364:2187–98.
Iung B, Cachier A, Baron G, et al. Decision-making in elderly patients with severe aortic stenosis: why are so many denied surgery? Eur Heart J. 2005;26:2714–20.
Charlson E, Legedza AT, Hamel MB. Decision-making and outcomes in severe symptomatic aortic stenosis. J Heart Valve Dis. 2006;15:312–21.
Leon MB, Smith CR, Mack M, et al. Transcatheter aortic-valve implantation for aortic stenosis in patients who cannot undergo surgery. N Engl J Med. 2010;363:1597–607.
Bouma BJ, van der Meulen JH, van den Brink RB, et al. Variability in treatment advice for elderly patients with aortic stenosis: a nationwide survey in The Netherlands. Heart. 2001;85:196–201.
Bach DS, Cimino N, Deeb GM. Unoperated patients with severe aortic stenosis. J Am Coll Cardiol. 2007;50:2018–9.
van Geldorp MW, van Gameren M, Kappetein AP, et al. Therapeutic decisions for patients with symptomatic severe aortic stenosis: room for improvement? Eur J Cardiothorac Surg. 2009;35:953–7.
Gibbons RJ, Balady GJ, Bricker JT, et al. ACC/AHA 2002 guideline update for exercise testing: summary article: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1997 Exercise Testing Guidelines). Circulation. 2002;106:1883–92.
Das P, Rimington H, Chambers J. Exercise testing to stratify risk in aortic stenosis. Eur Heart J. 2005;26:1309–13.
Otto CM. Valvular aortic stenosis: disease severity and timing of intervention. J Am Coll Cardiol. 2006;47:2141–51.
Iung B, Baron G, Butchart EG, et al. A prospective survey of patients with valvular heart disease in Europe: the Euro Heart Survey on Valvular Heart Disease. Eur Heart J. 2003;24:1231–43.
Hachicha Z, Dumesnil JG, Bogaty P, et al. Paradoxical low-flow, low-gradient severe aortic stenosis despite preserved ejection fraction is associated with higher afterload and reduced survival. Circulation. 2007;115:2856–64.
Lee DH, Buth KJ, Martin BJ, et al. Frail patients are at increased risk for mortality and prolonged institutional care after cardiac surgery. Circulation. 2010;121:973–8.
Robinson TN, Eiseman B, Wallace JI, et al. Redefining geriatric preoperative assessment using frailty, disability and co-morbidity. Ann Surg. 2009;250:449–55.
Head SJ, Bogers AJ, Serruys PW, et al. A crucial factor in shared decision making: the team approach. Lancet. 2011;377:1836.
Lim P, Monin JL, Monchi M, et al. Predictors of outcome in patients with severe aortic stenosis and normal left ventricular function: role of B-type natriuretic peptide. Eur Heart J. 2004;25:2048–53.
Reynolds MR, Magnuson EA, Lei Y, et al. Health-related quality of life after transcatheter aortic valve replacement in inoperable patients with severe aortic stenosis. Circulation. 2011;124:1964–72.
Pellikka PA, Sarano ME, Nishimura RA, et al. Outcome of 622 adults with asymptomatic, hemodynamically significant aortic stenosis during prolonged follow-up. Circulation. 2005;111:3290–5.
Acknowledgements
The authors would like to thank the patients and colleagues of the participating hospitals for their enthusiastic collaboration: Albert Schweitzer Ziekenhuis, Erasmus University Medical Center, Havenziekenhuis, Maasstad Ziekenhuis, Sint Franciscus Gasthuis, Vlietland Ziekenhuis, and IJsselland Ziekenhuis.
Conflict of interest
None declared.
Author information
Authors and Affiliations
Corresponding author
Additional information
Helena J. Heuvelman and Martijn W. A. van Geldorp have equally contributed to this work.
Appendix: Definitions
Appendix: Definitions
- Body surface area:
-
calculated with DuBois and DuBois formula.
- Carotid disease:
-
stenosis >50 %, or previous or planned surgery.
- Chronic obstructive pulmonary disease:
-
diagnosis previously made by physician, or receiving bronchodilators.
- Congestive heart failure:
-
hospital stay with clinical sign(s) of congestive heart failure.
- Coronary artery disease:
-
>50 % stenosis in at least one coronary artery proved by coronary angiography, or previously coronary artery bypass grafting.
- Diabetes:
-
diagnosis previously made by physician, or receiving blood glucose-lowering medication.
- Dyslipidaemia:
-
diagnosis previously made by physician, or receiving lipid-lowering medication.
- Hypertension:
-
diagnosis previously made by physician, or known blood pressure of ≥140 mmHg systolic or ≥90 mmHg diastolic on at least two measurements, or receiving blood pressure-lowering medication.
- Ischaemia:
-
ST depression ≥1 mm at J + 60 ms in at least two electrocardiographic leads.
- Left ventricular hypertrophy:
-
S in V1 plus R in V5/V6 > 35 mm, R in V6 > R in V5, R in I and/or aVL > 12 mm on electrocardiography at J + 60 ms.
- Myocardial infarction:
-
diagnosis previously made by physician.
- Peripheral arterial disease:
-
claudication, or previous or planned surgery of the lower limbs.
- Renal failure:
-
diagnosis previously made by physician or creatinine ≥200 μmol/l.
- Smoking:
-
smoking cigarettes or cigars for ≥5 years in the past.
- Stroke:
-
diagnosis ‘transient ischaemic attack’ or ‘cerebrovascular accident’ previously made by physician, or neurological disease severely affecting ambulation or day-to-day functioning.
Rights and permissions
About this article
Cite this article
Heuvelman, H.J., van Geldorp, M.W.A., Kappetein, A.P. et al. Clinical course of patients diagnosed with severe aortic stenosis in the Rotterdam area: insights from the AVARIJN study. Neth Heart J 20, 487–493 (2012). https://doi.org/10.1007/s12471-012-0309-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12471-012-0309-3