Abstract
Aims/hypothesis
We tested the hypothesis that dietary acid load may increase the risk of type 2 diabetes, and studied the association between acid load and insulin sensitivity as a possible mechanism involved.
Methods
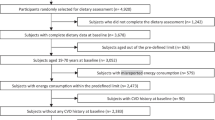
An observational survey with prospective follow-up including 911 non-diabetic Swedish men aged 70–71 years was carried out. The gold standard euglycaemic–hyperinsulinaemic clamp technique and the OGTT were used to determine insulin sensitivity and beta cell function, respectively. Diabetes incidence was assessed during 18 years of follow-up. Renal function was estimated from serum cystatin C concentrations. Dietary acid load was calculated as potential renal acid load (PRAL) and net endogenous acid production (NEAP) algorithms from 7 day food records. Adequate dietary reporters were identified by Goldberg cut-offs.
Results
PRAL and NEAP were not associated with insulin sensitivity or beta cell function. Underlying kidney function or consideration of dietary adequate reporters did not modify these null findings. During follow-up, 115 new cases of diabetes were validated. Neither PRAL nor NEAP was associated with diabetes incidence.
Conclusions/interpretation
Our results do not support the hypothesis that dietary acid load influences insulin sensitivity, beta cell function or diabetes risk. Interventional studies modifying acid–base dietary intake are needed to further elucidate a possible role of acid load in the development of type 2 diabetes.
Similar content being viewed by others
Abbreviations
- CVD:
-
Cardiovascular disease
- eGFR:
-
Estimated GFR
- IGI:
-
Insulinogenic Index
- IS:
-
Insulin sensitivity
- MUFA:
-
Monounsaturated fatty acid
- NEAP:
-
Net endogenous acid production
- PRAL:
-
Potential renal acid load
- PUFA:
-
Polyunsaturated fatty acid
- SFA:
-
Saturated fatty acids
- UAER:
-
Urinary albumin excretion rate
- ULSAM:
-
Uppsala Longitudinal Study of Adult Men
References
Tuomilehto J, Lindstrom J, Eriksson J et al (2001) Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Engl J Med 344:1343–1350
Knowler W, Barrett-Connor E, Fowler S et al (2002) Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 346:393–403
Fagherazzi G, Vilier A, Bonnet F et al (2014) Dietary acid load and risk of type 2 diabetes: the E3N-EPIC cohort study. Diabetologia 57:313–320
Pizzorno J, Frassetto LA, Katzinger J (2010) Diet-induced acidosis: is it real and clinically relevant? Br J Nutr 103:1185–1194
McAuley K, Mann J (2006) Thematic review series: patient-oriented research. Nutritional determinants of insulin resistance. J Lipid Res 47:1668–1676
Adeva MM, Souto G (2011) Diet-induced metabolic acidosis. Clin Nutr 30:416–421
Weickert MO (2012) What dietary modification best improves insulin sensitivity and why? Clin Endocrinol 77:508–512
Sung KC, Jeong WS, Wild SH, Byrne CD (2012) Combined influence of insulin resistance, overweight/obesity, and fatty liver as risk factors for type 2 diabetes. Diabetes Care 35:717–722
Remer T (2000) Influence of diet on acid-base balance. Semin Dial 13:221–226
Scialla JJ, Anderson CA (2013) Dietary acid load: a novel nutritional target in chronic kidney disease? Adv Chron Kidney Dis 20:141–149
Remer T, Dimitriou T, Manz F (2003) Dietary potential renal acid load and renal net acid excretion in healthy, free-living children and adolescents. Am J Clin Nutr 77:1255–1260
Frassetto LA, Todd KM, Morris RC Jr, Sebastian A (1998) Estimation of net endogenous noncarbonic acid production in humans from diet potassium and protein contents. Am J Clin Nutr 68:576–583
Remer T, Manz F (1994) Estimation of the renal net acid excretion by adults consuming diets containing variable amounts of protein. Am J Clin Nutr 59:1356–1361
Engberink MF, Bakker SJ, Brink EJ et al (2012) Dietary acid load and risk of hypertension: the Rotterdam Study. Am J Clin Nutr 95:1438–1444
Vessby B, Tengblad S, Lithell H (1994) Insulin sensitivity is related to the fatty acid composition of serum lipids and skeletal muscle phospholipids in 70-year-old men. Diabetologia 37:1044–1050
Byberg L, Zethelius B, McKeigue PM, Lithell HO (2001) Changes in physical activity are associated with changes in metabolic cardiovascular risk factors. Diabetologia 44:2134–2139
Larsson A, Malm J, Grubb A, Hansson LO (2004) Calculation of glomerular filtration rate expressed in mL/min from plasma cystatin C values in mg/L. Scand J Clin Lab Invest 64:25–30
DeFronzo RA, Tobin JD, Andres R (1979) Glucose clamp technique: a method for quantifying insulin secretion and resistance. Am J Physiol 237:E214–E223
Pollare T, Vessby B, Lithell H (1991) Lipoprotein lipase activity in skeletal muscle is related to insulin sensitivity. Arterioscler Thromb J Vasc Biol Am Heart Assoc 11:1192–1203
Seltzer HS, Allen EW, Herron AL, Brennan MT (1967) Insulin secretion in response to glycemic stimulus: relation of delayed initial release to carbohydrate intolerance in mild diabetes mellitus. J Clin Invest 46:323–335
Becker W (1994) Food habits and intake in Sweden 1989. The Swedish National Food Administration, Uppsala [in Swedish]
Willett WC, Howe GR, Kushi LH (1997) Adjustment for total energy intake in epidemiologic studies. Am J Clin Nutr 65:1220S–1228S, discussion 1229S-1231S
Resnick HE, Harris MI, Brock DB, Harris TB (2000) American Diabetes Association diabetes diagnostic criteria, advancing age, and cardiovascular disease risk profiles: results from the Third National Health and Nutrition Examination Survey. Diabetes Care 23:176–180
Goldberg GR, Black AE, Jebb SA et al (1991) Critical-evaluation of energy-intake data using fundamental principles of energy physiology: 1. Derivation of cutoff limits to identify under-recording. Eur J Clin Nutr 45:569–581
Lichtman SW, Pisarska K, Berman ER et al (1992) Discrepancy between self-reported and actual caloric intake and exercise in obese subjects. N Engl J Med 327:1893–1898
Cameron MA, Maalouf NM, Adams-Huet B, Moe OW, Sakhaee K (2006) Urine composition in type 2 diabetes: predisposition to uric acid nephrolithiasis. J Am Soc Nephrol 17:1422–1428
Maalouf NM, Cameron MA, Moe OW, Adams-Huet B, Sakhaee K (2007) Low urine pH: a novel feature of the metabolic syndrome. Clin J Am Soc Nephrol 2:883–888
Farwell WR, Taylor EN (2008) Serum bicarbonate, anion gap and insulin resistance in the National Health and Nutrition Examination Survey. Diabet Med 25:798–804
van den Berg E, Engberink MF, Brink EJ et al (2012) Dietary acid load and metabolic acidosis in renal transplant recipients. Clin J Am Soc Nephrol 7:1811–1818
Scialla JJ, Appel LJ, Astor BC et al (2011) Estimated net endogenous acid production and serum bicarbonate in African Americans with chronic kidney disease. Clin J Am Soc Nephrol 6:1526–1532
Jia T, Huang X, Qureshi AR et al (2014) Validation of insulin sensitivity surrogate indices and prediction of clinical outcomes in individuals with and without impaired renal function. Kidney Int. doi:10.1038/ki.2014.1
Acknowledgements
We are indebted to all participants in the study and are grateful to the ULSAM group for their assiduous and thorough data collection.
Funding
This work was supported by the grants from the Swedish Research Council and the Westman Foundation. Baxter Novum is the result of a grant from the Baxter Healthcare Corporation to Karolinska Institutet.
Duality of interest
BL is affiliated with Baxter Healthcare Corporation. All other authors declare that there is no duality of interest associated with their contribution to this manuscript.
Contribution statement
HX carried out the studies and data analyses and drafted the manuscript. JJC conceived the study, participated in its design and coordination, and helped to draft the manuscript. The other authors participated in its design and contributed to developing the manuscript to its final form. All authors approved the final version. JJC is guarantor of this work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xu, H., Jia, T., Huang, X. et al. Dietary acid load, insulin sensitivity and risk of type 2 diabetes in community-dwelling older men. Diabetologia 57, 1561–1568 (2014). https://doi.org/10.1007/s00125-014-3275-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-014-3275-z