Abstract
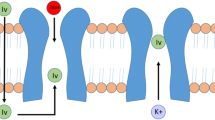
Introduction: Ivabradine is a heart rate-lowering agent that selectively inhibits the pacemaker current, If, in the sinoatrial node. The objective of this study was to evaluate the effects of a single intravenous administration of ivabradine on cardiac electrophysiological parameters in patients with normal baseline electrophysiology. The safety profile of ivabradine was also investigated.
Study design: This was an open-label, single-dose, non-controlled study conducted at one centre. Patients received a single dose of ivabradine (0.2 mg/kg) intravenously as a slow bolus over 15 seconds. Electrophysiological investigations, after catheter ablation for cardiac dysrhythmia, were performed at baseline and 30 minutes and 1 hour after drug administration. Electrode catheters were introduced and advanced to the right atrium, the bundle of His and the right ventricular apex of the heart. Electrophysiological parameters assessed included heart rate, QT interval, corrected QT interval (QTc), PR interval, sinoatrial conduction time, sinus node recovery time, and right atrial and ventricle refractory periods. Changes in electrophysiological parameters over time were assessed using one-way analysis of variance. In the case of a significant time effect, the Newman-Keuls procedure was used for comparison.
Patients: A total of 14 patients, 12 male and 2 female, aged 18–75 years were included in the study. The arrhythmia requiring catheter ablation was atrioventricular (AV) excitation in seven patients, paroxysmal supraventricular tachycardia in five patients, atrial fibrillation and flutter in one patient, and cardiac dysrhythmia in one patient. All patients had normal electrophysiology at baseline.
Results: Mean heart rate decreased significantly with ivabradine by 12.9 beats/min at 30 minutes and 14.1 beats/min at 1 hour. The mean QT interval increased but QTc showed no significant change from baseline. The PR and QRS intervals were unchanged. The right atrial and right ventricle refractory periods showed no significant change from baseline. The measured QT interval and the sinus node recovery time were increased. There were no clinically relevant changes in any other major electrophysiological parameters. Ivabradine was well tolerated and no serious adverse events occurred.
Conclusion: A single intravenous dose of ivabradine had a significant heart ratelowering effect, observed at 30 minutes and 1 hour after administration. Ivabradine did not prolong QTc or modify conductivity and refractoriness of the atrium, AV node, His-Purkinje system and ventricles, or repolarisation duration. These results confirm the action of ivabradine as a specific heart rate-lowering agent.


Similar content being viewed by others
References
Kannel WB, Kannel C, Paffenbarger RS, et al. Heart rate and cardiovascular mortality: The Framingham Study. Am Heart J 1987; 113: 1489–94
Hjalmarson Å, Gilpin E, Kjekshus J, et al. Influence of heart rate on mortality after acute myocardial infarction. Am J Cardiol 1990; 1: 547–53
Kjekshus J, Gullestad L. Heart rate as a therapeutic target in heart failure. Eur Heart J Suppl 1999; 1 Suppl H: H64–9
Anon. Management of stable angina pectoris: recommendations of the Task Force of the European Society of Cardiology. Eur Heart J 1997; 18: 394–413
Lechat P. Beta-blocker treatment in heart failure: role of heart rate reduction. Basic Res Cardiol 1998; 93 Suppl. 1: 148–55
Simon L, Ghaleh B, Puybasset L, et al. Coronary and hemodynamic effects of S 16257, a new bradycardic agent, in resting and exercising conscious dogs. J Pharmacol Exp Ther 1995; 275: 659–66
Pessina AC, Palatini P. Heart rate as a therapeutic target in hypertension. Eur Heart J Suppl 1999; 1 Suppl H: H70–5
Purcell H. Heart rate as a therapeutic target in ischaemic heart disease. Eur Heart J Suppl 1999; 1 Suppl. H: H58–63
Reneland R, Alvarez E, Andersson PE, et al. Induction of insulin resistance by beta-blockade but not ACE-inhibition: longterm treatment with atenolol or trandolapril. J Hum Hypertens 2000; 14: 175–80
Thollon C, Cambarrat C, Vian J, et al. Electrophysiological effects of S 16257, a novel sino-atrial node modulator, on rabbit and guinea-pig cardiac preparations: comparison with UL-FS 49. Br J Pharmacol 1994; 112: 37–42
DiFrancesco D. Characterization of single pacemaker channels in cardiac sino-atrial node cells. Nature 1986; 324: 470–3
DiFranceso D. The contribution of the “pacemaker” current (If) to generation of spontaneous activity in rabbit sino-atrial node myocytes. J Physiol 1991; 434: 23–40
Irisawa H, Brown HF, Giles W. Cardiac pacemaking in the sinoatrial node. Physiol Rev 1993; 73: 197–227
Bois P, Bescond J, Renaudon B, et al. Mode of action of bradycardic agent, S 16257, on ionic currents of rabbit sinoatrial node cells. Br J Pharmacol 1996; 118: 1051–7
Gardiner SM, Kemp PA, March JE, et al. Acute and chronic cardiac and regional haemodynamic effects of the novel bradycardic agent, S16257, in conscious rats. Br J Pharmacol 1995; 115: 579–86
Ragueneau I, Laveille C, Jochemsen R, et al. Pharmacokineticpharmacodynamic modeling of the effects of ivabradine, a direct sinus node inhibitor, on heart rate in healthy volunteers. Clin Pharmacol Ther 1998; 64: 192–203
Bazett JC. An analysis of time relations of electrocardiograms. Heart 1920; 7: 353–67
Malik M, Camm AJ. Evaluation of drug-induced QT interval prolongation. Drug Saf 2001; 24: 323–51
Malik M, Färbom P, Batchvarov V, et al. Relation between QT and RR intervals is highly individual among healthy subjects: implications for heart rate correction of the QT interval. Heart 2002; 87: 220–8
Toivonen L. More light on QT interval measurement. Heart 2002; 87: 193–4
The European Agency for the Evaluation of Medicinal Products. Committee for Proprietary Medicinal Products. Points to consider: the assessment of the potential for QT interval prolongation by non-cardiovascular medicinal products. CPMP/986/96. Available from URL: http://www.emea.eu.int int/pdfs/human/swp/098696en.pdf [Accessed 14 February 2003]
Kaneko A, Tachibana M. A voltage-clamp analysis of membrane currents in solitary bipolar cells dissociated from Carassius aureus. J Physiol 1985; 358: 131–52
Demontis GC, Longoni B, Barcaro U, et al. Properties and functional roles of hyperpolarization-gated currents in guinea-pig retinal rods. J Physiol 1999; 515: 813–28
Palatini P, Casiglia E, Pauletto P, et al. Relationship of tachycardia with high blood pressure and metabolic abnormalities: a study with mixture analysis in three populations. Hypertension 1997; 30: 1267–73
Palatini P, Julius S. Heart rate and the cardiovascular risk. J Hypertens 1997; 15: 3–17
Acknowledgements
Prof. Camm is supported by the British Heart Foundation.
This study was supported by IRIS (Institut de Recherches Internationales Servier).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Camm, A.J., Lau, CP. Electrophysiological Effects of a Single Intravenous Administration of Ivabradine (S 16257) in Adult Patients with Normal Baseline Electrophysiology. Drugs R&D 4, 83–89 (2003). https://doi.org/10.2165/00126839-200304020-00001
Published:
Issue Date:
DOI: https://doi.org/10.2165/00126839-200304020-00001